For a surgeon to effectively remove a non-palpable breast tumor, a radiologist must first mark its location and margins. Since the 1970s, the most common procedure used for this purpose has been wire localization: Radiologists place fine, thread-like wires near the tumor using a needle and image guidance. They remove the needle, leaving the wires extending outside the patient’s body. The wires are then taped to the skin to keep them in position while the patient is transported from the radiology suite to the surgical suite for tissue removal.
With wire localization, the radiology and surgical procedures must happen on the same day in the same facility, which creates scheduling challenges. Patients with exposed guidewires must be physically moved from the radiology suite to the surgical suite, and if a marker moves or is pulled out during transportation, there’s a risk that the surgeon may not remove the entire tumor. The procedure can also be an upsetting, uncomfortable procedure for patients who are already under significant stress.
An alternative existing procedure involves the radiologist placing small, radioactive seeds adjacent to the abnormal breast tissue to mark its location. The surgeon then uses a sterile Geiger counter to locate the seeds, facilitating tumor location for surgical excision. While this procedure eliminates the need for same-day procedures and the risk of shifting wires, the complex regulations associated with storing, tracking, and using radioactive seeds increases the burden on the hospital.
Health Beacons was founded in 2008 to develop a simpler, less-intrusive, precise approach to localizing the margins of non-palpable breast cancer tumors using radio-frequency identification (RFID) technology. Their vision was for the radiologist to implant miniature RFID tags using a needle and image guidance to delineate the tumor’s envelope. In surgery, the physician would then use a handheld device and probes with RFID sensors, which would locate the tags and guide the surgeon to the target tissue during dissection. When located, the reader would also present the tag’s unique ID number, so radiologists could provide the surgeon with information about the tumor’s location relative to each individual tag, which would improve accuracy during removal.
Without exposed guidewires, the patient could go home after placement of the RFID tags and return on the day of surgery, eliminating same-day scheduling challenges and reducing patient stress. And the use of precise RFID technologies could reduce the localization’s margin of error, which could also reduce the need for additional surgeries.
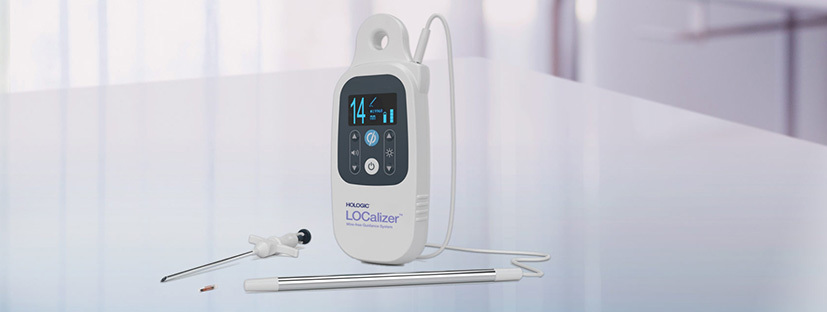
To realize their vision, Health Beacons’ founder hired Sunrise Labs, who engaged Sage for their medical device engineering and industrial design expertise to help bring what would eventually be called the LOCalizer™ from design to commercialization. Sage would design and develop the handheld reader and two probes: a large RFID probe integrated into the reader to identify gross tag location and a separate, single-use surgical probe, which plugs into the handheld reader, to pinpoint precise tag location during surgery. Sage also had the industrial design expertise needed to create an ergonomic, aesthetically pleasing form-factor and elegant user interface.